Skinny Fat: What It Really Means and How to Fix It
Published on: April 13, 2026
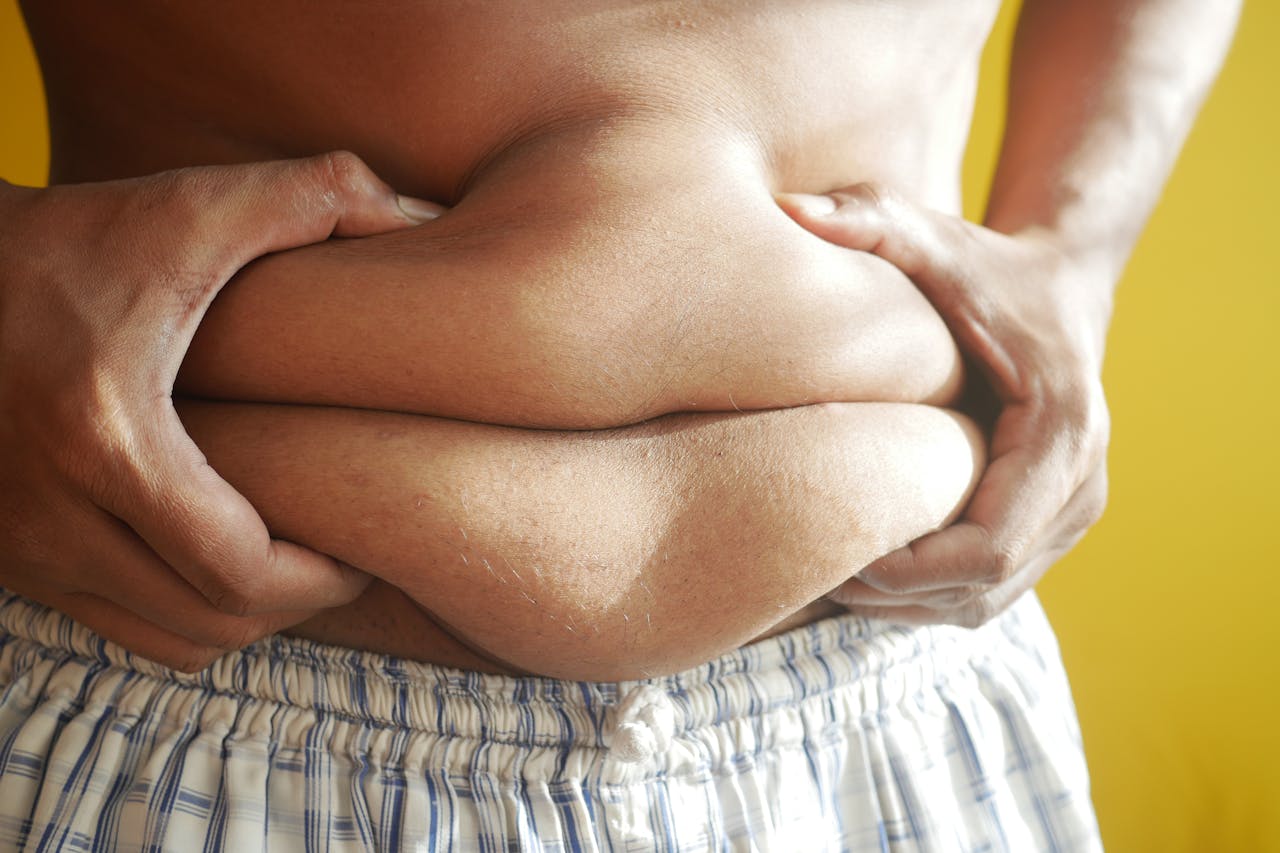
Your weight is normal. Your BMI says you're fine. But something doesn't quite add up — maybe your clothes fit differently, or you feel weaker than you'd expect, or your GP has flagged your blood sugar or cholesterol despite you not being overweight.
This is what people mean when they talk about being "skinny fat." It's not a medical diagnosis, but it describes something very real: a body that looks lean on the outside while carrying more fat and less muscle than is healthy on the inside.
And it's more common than most people think.
At a glance
- "Skinny fat" means having a normal weight but high body fat and low muscle mass — doctors call it metabolically obese, normal weight (MONW)
- BMI misses it completely because it doesn't distinguish between fat and muscle
- Visceral fat (the hidden kind around your organs) is the main health concern — it raises the risk of type 2 diabetes, heart disease, and metabolic syndrome
- Resistance training and adequate protein are the two most effective fixes, not cardio or calorie restriction
- People losing weight on GLP-1 medications need to be especially mindful of muscle preservation to avoid becoming skinny fat
What does skinny fat actually mean?
The medical term is "metabolically obese, normal weight" — MONW for short. It describes someone whose weight falls within the normal BMI range (18.5–24.9) but whose body composition tells a different story: too much body fat, particularly visceral fat, and not enough lean muscle mass.
BMI was never designed to measure body composition. It's a population-level screening tool that divides your weight by your height squared. It doesn't know — or care — whether that weight comes from muscle, fat, bone, or water. A person with a BMI of 22 could have a body fat percentage of 18% or 35%. Those are two very different metabolic pictures.
This is why someone can look slim in clothes, weigh what the charts say they should, and still have the metabolic markers of someone classified as obese: elevated fasting glucose, insulin resistance, high triglycerides, low HDL cholesterol. Research published in the Archives of Internal Medicine found that people with MONW who are over 65 have an elevated risk of cardiovascular death — despite their "normal" weight.
The disconnect between appearance and internal health is what makes this condition easy to miss and easy to dismiss.
How to tell if you're skinny fat
There's no single test, but several signs point in the same direction:
Body shape clues. A soft midsection despite being a normal weight is the most common visual sign. Fat accumulating around the belly — even when arms and legs stay relatively thin — suggests visceral fat storage. For women, a waist measurement above 80 cm (31 inches) increases metabolic disease risk. For men, the threshold is 94 cm (37 inches).
Low muscle tone and strength. If everyday tasks feel harder than they should — carrying shopping bags, climbing stairs, getting up from the floor — that may reflect low muscle mass rather than low fitness.
Blood markers. Your GP might flag elevated blood sugar, high LDL cholesterol, high triglycerides, or low HDL cholesterol. These metabolic red flags can appear at any weight.
Energy and endurance. Feeling unusually tired or breathless during moderate activity, despite not being overweight, can indicate poor body composition.
The most accurate way to assess this is a body composition scan — either a DEXA scan (available at some NHS trusts and private clinics) or a bioelectrical impedance analysis (BIA). These measure your actual body fat percentage and lean mass distribution, giving you information BMI simply can't.
Healthy body fat ranges are roughly 10–20% for men and 18–28% for women. If you're within a normal BMI but above these ranges, you're likely in skinny fat territory.
What causes it?
Several things can tip the balance toward more fat and less muscle, often working together.
Too little resistance training
This is the big one. Muscle is metabolically expensive tissue — your body will shed it if you don't give it a reason to keep it. Cardio alone doesn't provide that reason. Running, cycling, and swimming are excellent for cardiovascular health, but they don't stimulate the kind of mechanical loading that maintains or builds muscle mass. Without resistance training, muscle gradually declines — especially from your 30s onwards.
Poor diet quality (even at a normal calorie intake)
You don't have to overeat to become skinny fat. A diet heavy in ultra-processed foods, refined carbohydrates, and added sugar — even within a normal calorie range — promotes fat storage and provides poor building blocks for muscle. Low protein intake is particularly problematic: without sufficient amino acids, your body simply can't maintain lean tissue.
Prolonged or extreme calorie restriction
This catches people off guard. Crash diets and very low-calorie approaches often cause the body to break down muscle for energy, especially when protein intake is inadequate. You lose weight on the scales, but a disproportionate amount of that lost weight is muscle rather than fat. The result: a lighter version of yourself with a worse body composition than when you started.
Age-related muscle loss
Sarcopenia — the gradual loss of muscle mass with age — begins as early as your 30s and accelerates after 50. Without active effort to counteract it, you lose roughly 3–8% of your muscle mass per decade. Fat mass tends to increase over the same period, a double shift that worsens body composition even if your weight stays stable.
Hormonal changes
Menopause is a significant driver for women. Declining oestrogen promotes visceral fat storage (particularly around the abdomen) and makes it harder to maintain muscle. Thyroid dysfunction, chronically elevated cortisol from stress, and insulin resistance can all contribute too.
Genetics
Where your body stores fat and how easily you build muscle are partly genetic. Some people are more predisposed to carry visceral fat than subcutaneous fat (the kind you can pinch). This doesn't mean body composition can't be changed — it can — but it helps explain why two people with identical lifestyles can look and test very differently.
Why being skinny fat matters for your health
The concern isn't cosmetic. It's the visceral fat — the fat you can't see.
Visceral fat sits deep in the abdominal cavity, wrapping around your liver, kidneys, intestines, and pancreas. Unlike subcutaneous fat (the pinchable layer under your skin), visceral fat is metabolically active in ways that are harmful. It produces inflammatory chemicals and disrupts hormone signalling, contributing to insulin resistance, elevated blood pressure, and abnormal cholesterol levels.
Together, these factors constitute metabolic syndrome — a cluster of conditions that significantly raises your risk of type 2 diabetes, heart disease, and stroke. And because skinny fat people look normal on the outside, they're less likely to be screened for these issues by their GP.
Low muscle mass compounds the problem. Muscle is your body's primary glucose sink — it absorbs blood sugar after meals. Less muscle means less capacity to clear glucose from the bloodstream, which pushes you toward insulin resistance. Research in JAMA Network Open has also linked the combination of high fat mass and low muscle mass to cognitive decline.
The short version: being skinny fat carries many of the same metabolic risks as being overweight, but it's far less likely to be caught.
How to fix a skinny fat body
The goal is body recomposition — reducing fat while building or preserving muscle. This isn't the same as losing weight. In fact, your weight on the scales may barely change while your body composition transforms significantly. Here's what actually moves the needle.
Start resistance training
This is non-negotiable. The UK Chief Medical Officers' guidelines recommend resistance training on at least two days per week, and for good reason — it's the most effective stimulus for building and maintaining muscle mass.
You don't need a gym membership or an elaborate programme. Compound movements — squats, deadlifts, rows, presses, lunges — work multiple muscle groups and give you the most return for your time. Start with bodyweight or light resistance and build progressively. Consistency matters far more than intensity in the early weeks.
If you're new to strength training, even two sessions per week produces measurable improvements in lean mass within 8–12 weeks.
Prioritise protein
Muscle is built from protein, and most people don't eat enough of it — especially when trying to manage their weight. Aim for 1.2–1.6 g of protein per kilogram of body weight per day. For a 70 kg person, that's roughly 84–112 g daily.
Good sources include chicken, fish, eggs, Greek yoghurt, tofu, lentils, and beans. Spreading protein across the day (rather than loading it into one meal) supports better muscle protein synthesis. If you're struggling to hit your targets through food alone, protein shakes can help fill the gap. We've also compiled a list of high-protein, low-calorie foods for practical meal ideas.
Eat at maintenance or a slight deficit
Body recomposition works best when you're not in a steep calorie deficit. Severe restriction signals your body to conserve energy and break down muscle — exactly the opposite of what you need. Eating around your maintenance calories (or just slightly below) while increasing protein and training with resistance is the sweet spot.
Use your BMR as a starting point and adjust based on how your body responds over 2–4 weeks. If you're losing strength or feeling constantly drained, you're cutting too much.
Don't abandon cardio — just rebalance it
Cardio still matters for heart health, mood, and metabolic function. The issue is when it's all you do. If your current routine is five days of running and no strength work, shifting to three days of resistance training and two days of moderate cardio would be a better balance.
Walking is underrated. A daily 30-minute walk supports fat loss, improves insulin sensitivity, and doesn't interfere with muscle recovery the way long-duration cardio can.
Fix your sleep
Poor sleep disrupts the hormones involved in muscle repair and fat storage. Cortisol rises, growth hormone drops, and appetite-regulating hormones (leptin and ghrelin) shift in favour of overeating. Seven to nine hours of quality sleep per night isn't a luxury — it's a fundamental part of body recomposition.
Address underlying hormonal issues
If you suspect hormonal factors — perimenopause, thyroid dysfunction, chronic stress — talk to your GP. Blood tests can identify treatable causes that might be working against your efforts. Fixing an underactive thyroid or managing cortisol won't transform your body overnight, but it removes a significant barrier.
A note for people on GLP-1 medications
This is something we see increasingly, and it's worth flagging.
GLP-1 medications like Mounjaro (tirzepatide) and Wegovy (semaglutide) are powerful tools for weight loss. But any rapid weight loss — whether from medication, surgery, or severe dieting — carries a risk of losing muscle alongside fat. If you're on a GLP-1 and not actively protecting your lean mass, you can end up lighter but with a worse body fat-to-muscle ratio than when you started. In other words: skinny fat.
The fix is straightforward but requires intention:
Eat enough protein. This matters even more on GLP-1 medications because your appetite is suppressed, so total food intake drops. Make sure what you do eat is protein-rich — at least 1.2 g per kg of your target body weight daily.
Train with resistance. Even two sessions per week signals your body to hold onto muscle while shedding fat.
Don't rush the titration. Slower, steadier weight loss tends to preserve more lean mass than rapid drops.
We've written a full guide to preserving muscle on GLP-1 medications that goes deeper into the practical strategies.
When to see your GP
If you recognise the skinny fat pattern in yourself — normal weight but a soft midsection, low energy, family history of diabetes or heart disease — it's worth having a conversation with your GP. Ask about:
- Fasting blood glucose and HbA1c (to screen for insulin resistance and prediabetes)
- A lipid panel (cholesterol and triglycerides)
- Blood pressure
- Waist circumference measurement
- Thyroid function, if you have other symptoms suggesting an underactive thyroid
These are standard tests, and your GP can run them as part of an NHS Health Check (available to everyone aged 40–74 in England). If results flag metabolic concerns, early intervention — through lifestyle changes and, where appropriate, medical support — can make a significant difference.
The bottom line
Being skinny fat means your weight looks fine on paper while your body composition tells a different story. The risks — metabolic syndrome, insulin resistance, cardiovascular disease — are real and often undetected. The fix isn't about losing weight; it's about changing what your weight is made of. Resistance training, adequate protein, and sustainable habits matter far more than the number on the scales.
This article is for informational purposes only and does not constitute medical advice. Always consult with a qualified healthcare professional before starting any treatment.